Photophobia is a signal, not a personality trait
Light sensitivity can come from the surface (tear film, cornea) or from deeper inflammation. A quick look may not capture the difference.
A narrative about sudden eye pain with light exposure, why early reassurance can be misleading, and what changes when the right tests are performed. Names have been changed for privacy.
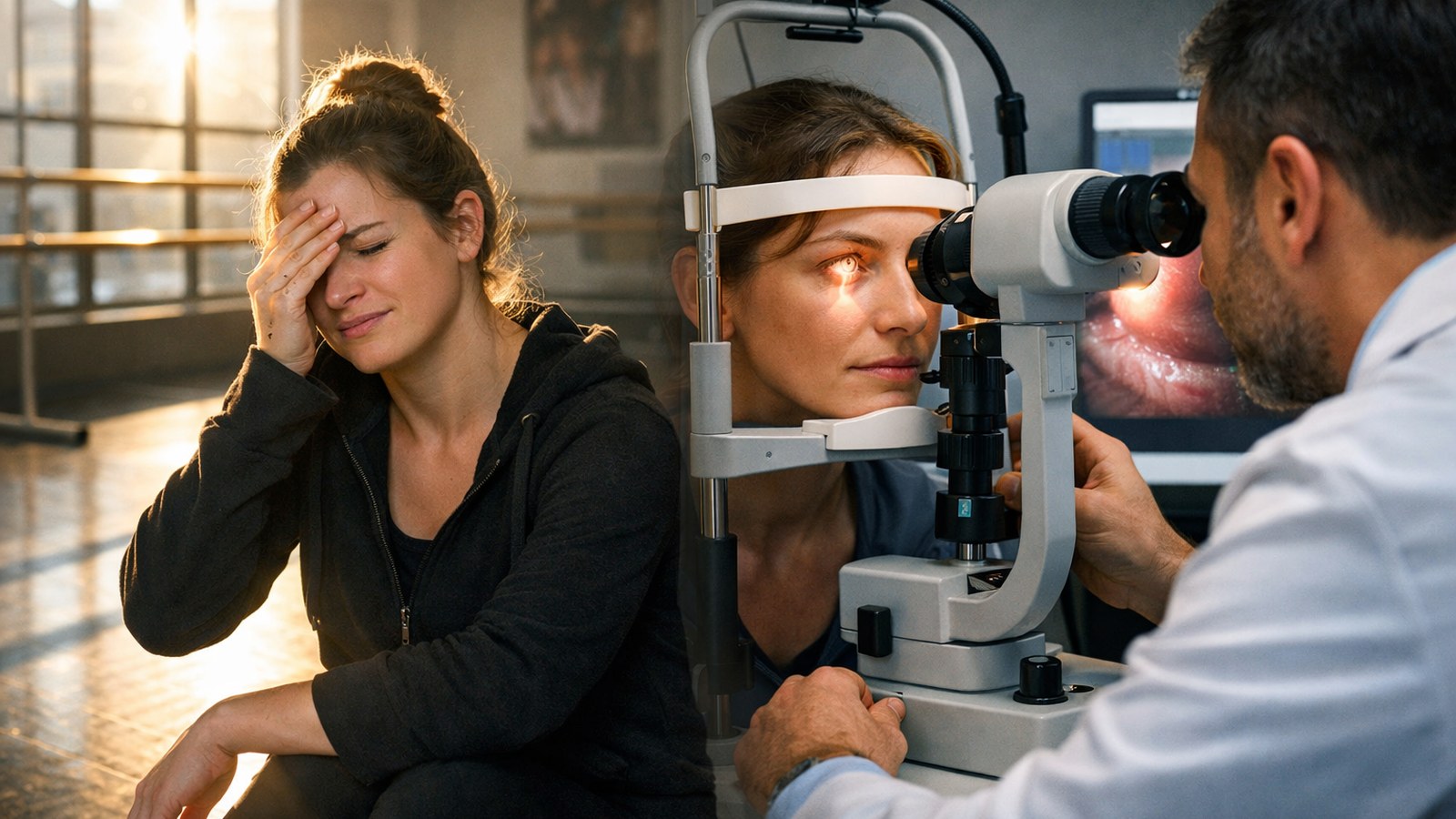
A normal morning becomes a problem when light itself feels sharp.
Stephanie had the kind of schedule that trained her to ignore minor discomfort. She worked the front desk at a dance studio, filled in for classes when an instructor got stuck in traffic, and spent her evenings answering parent emails about recital costumes. In Provo, Utah, the morning sun could be bright even in colder months, and the studio’s lobby had big windows that made the floor look like it had been polished with light.
That morning, the brightness felt different. It was not just squinting. It was pain, a thin, immediate sting that seemed to originate deeper than the surface. When she walked past the windows, her right eye clamped shut on reflex. The sensation surprised her because she had woken up feeling normal. No gritty dryness. No major redness. No memory of rubbing her eye too hard.
She tried to keep the day moving. She grabbed the studio keys, walked inside, and turned on the front lights. The overhead fixtures, usually unremarkable, made the pain spike. It was as if the light had weight. It pressed. She could still see, but her vision felt less cooperative, like it needed extra effort to stay clear.
A parent arrived early to ask about a schedule change. Stephanie kept her right eye angled away and hoped no one would notice. When she looked at the computer screen to check the calendar, she felt another sharp pulse. Her eye watered, which made it look like she was emotional rather than uncomfortable. The mismatch annoyed her. She did not feel dramatic. She felt precise pain.
By midmorning she had started doing small calculations. If it was a scratch, it would probably feel gritty. If it was allergies, she would probably itch. If it was a migraine, she would probably have the rest of the migraine. None of that fit. She put on sunglasses indoors, which felt ridiculous, but it lowered the intensity enough that she could keep her eye open.
At lunch she stepped outside and the winter sun hit her face. She flinched hard enough that she had to stop walking. That was the moment she accepted she was not being cautious. She was reacting to something that had changed.
When symptoms are real but the exam is brief, the story can stall.
She chose the fastest appointment available, a walk-in clinic near the studio. She explained the problem in the simplest terms she could: “Light hurts. It feels sharp. It is worse in my right eye.” She expected an immediate plan, something that matched the urgency of the sensation.
The provider looked at her eye with a small handheld light, asked if she wore contacts, and listened to her describe the timeline. Stephanie said no contacts. She said no major injury. She said she had not been sick recently, although she had been tired, which was a constant state for someone who worked around dancers and their parents.
The provider asked her to follow a finger, then looked again at the eye from arm’s length. “I do not see anything,” the provider said. “It might be irritation. Maybe a little dryness. You can use lubricating drops. If it gets worse, see an eye doctor.”
The phrase “I do not see anything” landed like a verdict. Stephanie wanted to trust it. Quick reassurance has its own gravity. It tells the nervous system to stand down. It tells the mind to stop investigating. It implies that the pain is either temporary or exaggerated.
She left with a small bag of drops and a sense of being slightly embarrassed. Nothing was wrong, which meant she had overreacted. On the drive back to the studio, she tried to treat the pain like a nuisance rather than a warning. She repeated the provider’s language in her head: irritation, dryness, nothing.
But pain with light exposure does not always behave like a simple nuisance. That afternoon, when she stood near the mirrored wall in the studio and watched a class warm up, the reflections triggered discomfort again. She noticed her eye looked mildly red now, not the dramatic red of a burst blood vessel, more like a subtle flush around the colored part of the eye. She also noticed that the pain felt worse when she tried to focus close, like reading a text message.
She used the drops. They helped for a few minutes in the way that any cool liquid can help. Then the pain returned, unchanged in character. It was not a scratchy surface pain. It was a deep ache with a sharp edge.
That evening she left the studio and drove home with the car’s interior lights dimmed. When headlights from oncoming traffic hit the windshield, she felt her right eye tighten. She started thinking in a different direction, not about dryness but about what she would do if she woke up the next day and it was worse.
A symptom that persists is not a character flaw. It is data.
Stephanie did not enjoy being persistent. She had been raised to be polite and to not take up too much space. The walk-in visit had given her a narrative that she was trying to honor: it was minor, it would pass, she just needed rest.
But during a late class, a student asked her why she was wearing sunglasses indoors. Stephanie laughed it off, then realized she could not keep laughing it off. She had been protecting her eye all day, and it had not improved. If anything, it felt more reactive. When she blinked, it felt as if the eye was swollen on the inside.
She went home and did what nearly everyone does now. She searched the symptom. She found lists that ranged from mild to terrifying. She found phrases like “photophobia” and “uveitis” and “keratitis.” She also found reassuring explanations that suggested stress, migraines, and dry eye. The internet did what it always does: it offered both comfort and fear, sometimes in the same paragraph.
What she did not find was a satisfying explanation for why a clinician could say nothing was wrong while her eye responded to light like it was being scraped. That gap made her realize she needed a different kind of exam.
The next morning, she scheduled a same-day appointment with an eye specialist. She chose a practice that listed urgent visits and advanced imaging on its website, partly because she needed the psychological permission of a clinic that treated “eye pain” as a legitimate reason to be seen quickly.
At the desk she said the words that now felt important to say out loud: “Pain with light. It is new. It is persistent.” The staff did not react dramatically. They just moved her through the intake process like they had heard the story before. That calm competence felt like relief.
A deeper evaluation is not about fancy gadgets. It is about seeing the right structures.
The specialist started with history, but it was a different kind of history. Instead of asking only “What happened,” she asked “What is the pattern.” Does the pain worsen when light hits the other eye too. Is the vision blurry or just harder to keep stable. Is there tearing. Any recent cold sores. Any autoimmune history in the family. Any back pain that feels inflammatory. The questions were precise and oddly comforting. They implied a map.
Then came the measurements: visual acuity, pupil responses, pressure, and a careful look at the surface with dye and blue light. Stephanie had expected the dye test at the walk-in clinic. She had not gotten it. Here, it was routine. The specialist watched the tear film and the corneal surface like she was reading a language.
“Surface looks mostly intact,” the specialist said. “That is good. But the symptom you described makes me want to look deeper.”
The slit lamp exam was the turning point. Sitting at the microscope, Stephanie tried to hold still while a narrow beam of light moved across her eye. The light was uncomfortable, but it was a controlled discomfort. It came with information. The specialist adjusted angles, changed magnification, and watched the front chamber, the space between the cornea and the iris.
“There are inflammatory cells,” she said, almost to herself. “And a little flare.”
Stephanie did not know what that meant, but she heard the key phrase: there is something. Not nothing. Not irritation. Something visible, structural, measurable. The specialist explained it in plain language: inflammation inside the eye can cause light sensitivity and pain because the iris and nearby structures are reacting, and light triggers the pupil to move, which can hurt.
They dilated her pupil and examined the back of the eye. They also did imaging, including photographs and a scan to ensure there were no subtle changes in the retina and optic nerve that would change the urgency or the differential. The process felt thorough but not theatrical. It was a sequence of checks that answered specific questions.
“This looks like anterior uveitis,” the specialist said. “Some people call it iritis.”
Stephanie felt a strange mix of fear and relief. Fear because the word sounded serious. Relief because the symptom finally had a name, and names come with plans.
A label matters most when it explains what happens next.
The specialist was careful about tone. She did not turn the diagnosis into a cliffhanger. She explained that uveitis is a category, not a single disease. Sometimes it is associated with an underlying autoimmune condition. Sometimes it occurs after an infection. Sometimes, even after a careful workup, the cause remains unclear.
What mattered in the room was that the inflammation was treatable and that delaying treatment could increase risk of complications. She explained the near-term goals: reduce inflammation, control pain, prevent the iris from sticking to the lens, and monitor pressure.
The treatment plan included prescription drops designed to calm inflammation and another medication to relax the focusing system and reduce painful spasm. The specialist described the expected timeline, the need for follow-up, and what changes would trigger an urgent call back. She also described side effects Stephanie might notice, including blurry near vision from dilation-like effects, and why those effects were part of the plan rather than a sign of failure.
There was also a second layer to the plan: a limited set of tests to check for associated systemic conditions if the inflammation recurred or if the exam suggested a broader pattern. The specialist explained that not every first episode requires a full laboratory panel, but that patterns over time can guide the decision. The message was balanced. It acknowledged uncertainty without dismissing the symptom.
Stephanie asked the question she had been holding since the walk-in visit. “How could they not see this?”
The specialist did not criticize the first provider. She framed it as a mismatch of tools and context. Without a slit lamp exam, without looking specifically for inflammatory cells, and without measuring the right features, the eye can appear nearly normal from a distance. The redness can be subtle. The pain can be out of proportion to what a general exam reveals.
“You were not wrong to come in,” the specialist said. “Pain with light is one of those symptoms that deserves a careful look.”
Relief can be gradual. So can the emotional reset.
On the first day of treatment, Stephanie did not feel instantly cured. The pain softened in steps rather than disappearing. That made sense once she understood the mechanism. Inflammation is not a switch. It is a process. The eye is small but complex, and its tissues react on their own timeline.
She took time off from teaching that week. Not because the specialist insisted, but because her eye needed a quieter environment while it stabilized. The dance studio, with its mirrors and bright overhead lights, had been a constant trigger. She was relieved to step away and let the symptom settle instead of repeatedly testing her tolerance.
After two days, she could walk through her living room with curtains open without the immediate flinch response. She still noticed brightness, but it no longer felt like pain had replaced light. By day four, she could read without feeling as if her eye was arguing with the task.
The follow-up appointment mattered as much as the first. The specialist rechecked the same landmarks, measured pressure again, and confirmed that the inflammatory signs were decreasing. Stephanie learned a new kind of trust, not the blind trust of reassurance, but the grounded trust of repeated measurement.
She also learned something about herself. She had interpreted persistence as a personal flaw. She had thought that seeking a second opinion was a form of being difficult. The experience corrected that. Persisting was not being difficult. Persisting was being accurate.
What this story is meant to illustrate.
Light sensitivity can come from the surface (tear film, cornea) or from deeper inflammation. A quick look may not capture the difference.
The turning point was not a single machine. It was a structured exam: slit lamp evaluation, careful dilation, and targeted imaging.
A second clinician may use different tools and ask different questions. That can change the diagnosis, not because someone was careless, but because the context is different.
Next reads that connect to care navigation and modern testing.
What OCT shows, why trends matter, and how it shapes monitoring.
Records, framing questions, and comparing plans when decisions are high impact.
Brightness, glare, and behavior often matter more than specialty lenses.