What is being changed
Cornea reshaping, lens replacement, retinal fluid control, or pressure lowering. If you cannot describe the mechanical change, you are vulnerable to marketing language.
What each procedure changes, what it treats, the tradeoffs, and the recovery realities.

The useful version of a procedure includes candidacy, alternatives, outcomes you can measure, and the realistic list of risks and recovery constraints.
Procedures are often described as a single event. In real care, they are part of a workflow: a diagnosis or problem statement, a candidacy evaluation, a plan tailored to anatomy and goals, a recovery period, and follow up monitoring. The same procedure name can produce different experiences depending on the baseline condition, ocular surface health, and the definitions of success used by the patient and clinician.
Most eye procedures fall into a few categories. Refractive procedures change how the eye focuses by reshaping the cornea or changing lens optics. Lens procedures replace the natural lens or modify its performance. Retina procedures treat macular and vascular disease and are often schedule dependent. Glaucoma procedures reduce risk of optic nerve damage progression, usually by lowering eye pressure. Cornea and surface procedures range from symptom control to structural vision restoration.
A procedure is a tool. The right tool depends on goals, anatomy, and risk tolerance.
A practical way to evaluate any eye procedure is to separate four layers. First is the underlying problem being treated. Second is the mechanism, meaning what physical change is being made. Third is the outcome definition, meaning what success looks like in measurable terms. Fourth is the tradeoff set, meaning what side effects are acceptable and which are not.
Many misunderstandings happen because people focus on one metric, usually visual acuity, while ignoring contrast, glare, dryness, or stability over time. A procedure can improve one axis while worsening another. The best consults make those axes explicit.
Cornea reshaping, lens replacement, retinal fluid control, or pressure lowering. If you cannot describe the mechanical change, you are vulnerable to marketing language.
Visual acuity is one metric. Others include contrast sensitivity, night driving function, glare and halos, dependence on glasses, stability of results, and the need for ongoing treatments.
Glasses, contacts, drops, monitoring, or different procedures. Timing matters because candidacy and risk can change over time, especially with cataract progression or ocular surface instability.
If your challenge is referrals, records, scheduling, or evaluating multiple opinions, see Care Guide.
Lens replacement that restores clarity and often changes glasses dependence.
Cataract surgery replaces the natural lens with an artificial intraocular lens (IOL). The clinical goal is restoring clarity and function when lens aging reduces contrast and increases glare. In modern practice, cataract surgery also includes a refractive decision: whether to prioritize distance vision, near vision, or a blended strategy, and whether to address astigmatism at the same time.
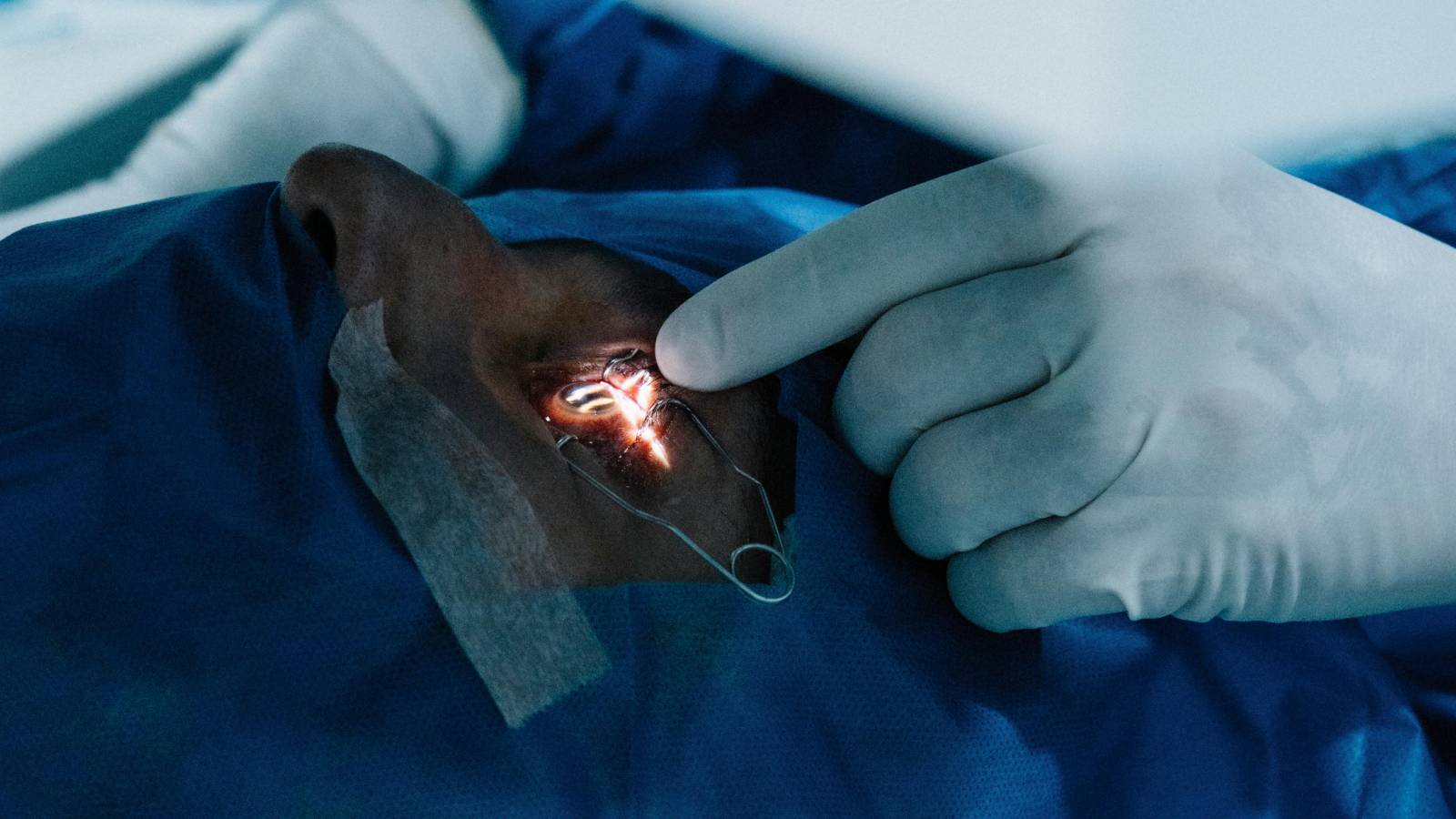
Cataracts are common, but the timing of surgery is individualized. The question is not simply whether a cataract exists. The useful question is whether it is limiting function enough that the benefits outweigh the risks and inconvenience now. Functional limitation can mean night driving glare, reduced contrast, difficulty reading in dim light, or overall visual quality that is not corrected by glasses.
Monofocal lenses usually prioritize one distance. Toric lenses address astigmatism. Multifocal and extended depth of focus lenses can reduce reading glasses dependence for some people, but may increase glare or halos for some tasks and lighting conditions.
Many people improve quickly, but vision can fluctuate during healing. Drops and follow up visits are standard. If both eyes need surgery, timing between eyes is part of planning.
Cornea reshaping procedures where candidacy is the main filter.
LASIK and PRK are refractive procedures that reshape the cornea to change how light focuses. They can reduce dependence on glasses for selected candidates, but outcomes depend on preoperative anatomy and surface health. Screening is not a formality. It is how risk is managed.
Candidacy commonly depends on corneal thickness and shape, prescription stability, pupil size in low light, and ocular surface status. Dry eye risk matters because reduced tear stability can degrade quality even if visual acuity is good. Some people can read the chart but do not like how their vision feels.
Reduced need for distance glasses in daily life. Some people still need glasses for specific tasks, and many people will still need reading correction with age.
Dryness symptoms, glare and halos, and the difference between high contrast chart vision and real world visual quality. The risk profile varies with prescription and anatomy.
The tear film is the first optical surface. If it is unstable, vision can fluctuate and comfort can decline even when refraction is accurate. See Digital Life and Habits.
Injections, lasers, and surgery, typically for disease management rather than comfort.
Retina treatments are used for macular disease, diabetic retinopathy, and retinal vascular problems. Many modern protocols include anti VEGF injections, which reduce abnormal blood vessel activity and leakage in certain conditions. Some conditions also use steroid injections or implants. Laser is used in specific scenarios, and retinal surgery is used for problems like retinal detachment and certain macular interface disorders.
Success in retina care is often defined as preserving function and preventing progression. In many diseases, the realistic goal is stability rather than perfection. This is also why follow up schedules matter. Retina care can be time and visit intensive when a condition is active.
Abnormal vessel growth and leakage in certain macular conditions. Outcomes depend on diagnosis, baseline damage, and how early treatment began.
Many protocols are schedule dependent. Symptoms can feel stable while active disease continues, so monitoring and timing are part of the treatment.
Diabetes and vascular risk factors strongly influence retina outcomes. See Nutrition for the long view on risk.
For a deeper explainer, see Retina injections in plain language.
Options that lower eye pressure and reduce progression risk, including laser and MIGS.
Glaucoma is managed to reduce the risk of optic nerve damage progression, often by lowering intraocular pressure. Drops are common, but laser and surgical options exist. Some people use laser early to reduce dependence on drops. Others use procedures when pressure remains above target despite medications.
A key concept is the target pressure. Many glaucoma plans define a pressure goal based on optic nerve appearance, visual fields, corneal thickness, and risk factors. Procedures are often chosen when reaching the target pressure with drops alone is not realistic or not tolerated.
Selective laser trabeculoplasty is commonly used in open angle glaucoma and ocular hypertension. It aims to improve fluid outflow and lower pressure. Effect size and duration vary, and repeatability depends on the case.
Minimally invasive glaucoma surgery refers to a family of procedures often combined with cataract surgery in selected patients. The goal is usually modest pressure reduction with a favorable safety profile, not maximum pressure lowering in advanced disease.
Glaucoma outcomes are judged over time using pressure, optic nerve imaging, and visual fields. A procedure changes the pressure plan, but follow up monitoring remains the main protection against silent progression.
A wide category that spans symptom control, vision restoration, and structural repair.
The ocular surface includes the cornea, eyelids, tear film, and supporting glands. Surface problems are common because the system is exposed to air, friction, and environmental stress. Some procedures aim to improve tear stability and reduce inflammation. Others address corneal scars, irregularity, or transplant needs.
A useful way to think about surface interventions is to separate symptom relief from structural repair. Many treatments improve comfort and stability but do not permanently change anatomy. Structural procedures are used when the cornea itself is damaged, irregular, or failing.
Tear instability can cause fluctuating blur that improves with blinking. People sometimes interpret this as a need for a stronger prescription, but the driver is the surface, not the lens power.
Common categories include eyelid margin treatments, gland expression approaches, punctal occlusion in selected cases, and anti inflammatory strategies. The right plan depends on the driver and exam findings.
When the cornea is irregular or scarred, management may include specialty contacts, crosslinking in specific diseases, or transplant approaches. These are diagnosis specific and require careful follow up.
If your main complaint is burning, fluctuating blur, or screen intolerance, you may be in the surface category even if you can read the chart well. A focused evaluation of tear film stability and eyelid margin health is often a high value starting point.
Convert a sales pitch into a clinical decision with clear decision points.
The goal of consult questions is not confrontation. It is clarity. A good consult ends with a plan that defines what is being treated, what will change, how outcomes will be measured, and what happens if expectations are not met.
For visit preparation, records, and second opinion strategy, see Care Guide.
Short answers with enough context to be useful.
No. Procedures are tools with benefits and risks. In many scenarios, conservative options are best until function is limited or disease progression risk changes the equation.
Because anatomy and baseline surface health strongly predict outcomes. Screening is risk management. It helps match the right procedure to the right patient and avoids predictable failure modes.
Choosing based on one headline benefit, such as no glasses, without defining acceptable tradeoffs for night vision, dryness, reading needs, and recovery constraints.